Initial experience of robotic intersphincteric resection for rectal cancer
Article information
Trans Abstract
Purpose:
Robotic systems (the da Vinci Surgical System) may offer considerable advantages, particularly in rectal surgery operated in the confined pelvis. This study was carried out on the assumption that a robotically naive, yet laparoscopically experienced surgeon successfully transferred to a robotic environment. We assessed immediate surgical outcomes of robotic intersphincteric resection (ISR) as an initial experience of a single surgeon.
Methods:
We analyzed the data of 19 consecutive patients with rectal cancer who underwent robot ISR between January 2009 and March 2012. Its immediate surgical outcomes were compared with those of 19 patients who underwent laparoscopic ISR as a control group of the same cohort.
Results:
There was no significant difference in the mean operating time between robotic and laparoscopic group (261.6±57.7 minutes, 222.37±68.2 minutes, P=0.064). Mean distal resection margin was 1.5±2.2 and 1.1±0.9 in robotic and laparoscopic groups, respectively (P=0.464). Three patients in each group had a circumferential margin clearance of less than 1 mm. Two patients in each group suffered from anastomotic leakeage. There were no significant differences in date of flatus passage and dietary intake, and the length of postoperative hospital stay between both groups.
Conclusion:
Robotic ISR is a safe and feasible procedure and its early short-term surgical outcomes are comparable to those of laparoscopic surgery.
INTRODUCTION
Robotic systems (the da Vinci Surgical System, Intuitive Surgical Inc., Sunnyvale, CA, USA) have been adopted in various surgical fields such as urologic and gynecologic procedures with good results [1]. Robotic colorectal surgery was first performed in 2001 [2]. Robotic systems have several advantages over conventional laparoscopic surgery such as three-dimensional magnified vision, a surgeon-controlled camera and operating platform, articulating instruments with various degrees of freedom, excellent ergonomics and tremor filtration [3,4]. These technical benefits of robotic systems enable a surgeon to construct a stable and fine dissection space in the narrow and deep pelvic cavity [3,5].
As with any new surgical technique, however, there is an related learning curve. This learning curve includes operative outcomes and oncological outcomes. This study was conducted under the assumption that experienced laparoscopic surgeon could overcome the learning curve for robotic surgery quickly and easily. In this study, we compared operative and pathologic outcomes of robotic surgery at an early period with those of laparoscopic surgery at a late period of a single surgeon.
METHODS
We retrospectively analyzed immediate surgical outcomes of the 19 patients undergoing robotic intersphincteric resection (ISR) compared with those of 19 patients undergoing laparoscopic ISR for rectal cancer as a control group of the same cohort. All operations were performed by a single surgeon who has performed laparoscopic colorectal surgery more than 300 cases. These rectal cancer surgeries were performed between January 2009 and March 2012 at Kyung Hee University Medical Center. Data were collected in a prospectively maintained database that was further supplemented by retrospective chart review.
Surgical techniques
Under the general anesthesia, the patient was placed in modified lithotomy position by using Allen’s stirrups. All laparoscopic surgery and robotic surgery were executed in the order of 1) ligation of the inferior mesenteric vessels, 2) left colonic mobilization, 3) pelvic dissection, 4) intersphincteric dissection, 5) rectal reconstruction, and 6) ileostomy creation. For laparoscopic group, steps 1-4 were performed using a laparoscopic approach. For robotic group, whereas, steps 1-2 were performed using a laparoscopic approach and steps 3-4 using a robotic approach. Coloanal anastomosis was performed via a hand-sewn end to end manner with absorbable interrupted sutures. Finally, a loop ileostomy was created in the area of the right lower quadrant.
Outcome assessment
Patient factors and demographics were assessed including age, sex, body mass index, American Society of Anesthesiologists (ASA) score, history of previous abdominal surgery, tumor location from anal verge, tumor size, pathologic stage and preoperative concurrent chemoradiation therapy (CCRT).
Perioperative factors were compared of including operating time, transfusion rate and conversion rate. Oncologic adequacy was assessed including the number of harvested lymph nodes (LNs) and status of resection margins (distal, proximal, and circumferential margins).
Postoperative results included days to passing first flatus, resuming diet, the length of hospital stay and postoperative morbidity. Morbidity was defined as operation related complications including anastomotic leakage, paralytic ileus, wound problem, pulmonary problem, voiding difficulty and adjacent organ injury during surgery.
Statistical analysis
Data were analyzed using the PASW ver. 18.0 (SPSS Inc., Chicago, IL, USA). Continuous variables were used to derive the mean±SD and were tested for statistical significance using the Student’s t-test. Proportions were evaluated using chi-square test or Fisher’s exact test. A P-value of less than 0.05 was considered significant.
RESULTS
General characteristics of the patients were presented in Table 1. Robotic and laparoscopic groups were similar in terms of age, sex, BMI, ASA score, history of previous abdominal surgery, tumor location from anal verge, tumor size, tumor-node-metastasis (TNM) classification and the number of patients who received preoperative CCRT. The distribution of pathologic stage did not differ between the two groups (P=0.426).
Table 2 summarized perioperative outcomes. Operating time did not differ between robotic and laparoscopic group (261.6±57.7 minutes, 222.37±68.2 minutes, P=0.064). Conversion to open surgery was necessary in one patient of laparoscopic group, because tumor size was too big (17.5×9 cm) to perform a dissection in a relatively narrow pelvic space. Additionally, frozen biopsy showed distal resection margin was invaded. Consequently, this patient was performed abdominoperineal resection (APR). In robotic group, however, one patient was converted to laparoscopic surgery due to a collision between robotic arms. One patient required perioperative blood transfusion in each group. Protective stoma was performed for all patients in robotic and laparoscopic group. Mean distal resection margin was 1.5±2.2 and 1.1±0.9 in robotic and laparoscopic groups, respectively (P=0.464). Three patients in each group had a circumferential margin clearance of less than 1 mm (P=1.000). Mean number of LNs harvested was 12.0±3.9 and 15.7±6.3 in robotic and laparoscopic groups, respectively (P=0.033).
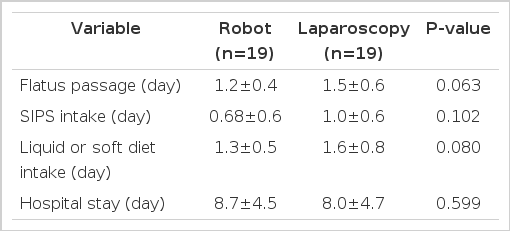
Outcomes of postoperative recovery were presented at Table 3. There were no significant differences in date of flatus passage, time to resume diet, and the length of postoperative hospital stay between both groups.
Overall operation-related complication was not different between the two groups (3 patients in robotic group and 6 patients in laparoscopic group, P=0.379) (Table 4). Two patients in each group suffered from anastomotic leakeage. In laparoscopic group, one patient with anastomotic leakage required percutaneous drainage. The others were treated with antibiotics. In robotic group, one patient injured the branch of inferior mesenteric vein by a trocar port, which was managed well by electrocautery and hem-o-lok clips (Non-absorbable Polymer Ligating Clips, Teleflex Medical, Research Triangle Park, NC, USA). In laparoscopic group, one patient with wound infection and one patient with postoperative paralytic ileus were treated conservatively. In laparoscopic group, two patients who had voiding difficulty were necessary to learn how to perform clean intermittent catheterization and these patients regained self-urination during outpatient follow-up. Operative mortality was none in both groups.
DISCUSSION
ISR has been used to extend the opportunity for sphincter preservation in patients with low rectal cancer. Several studies reported the comparison between open and laparoscopic ISR for low rectal cancer [6-9]. Compared with open ISR, laparoscopic ISR is a feasible procedure in respect of sphincter saving and morbidity without compromising the oncological benefits [7,8]. The laparoscopic procedure for low rectal cancer, however, requires advanced skill and considerable experience for precise dissection in the pelvic space. The learning curve for laparoscopic rectal surgery was considered difficult to overcome [3,10,11].
Robotic systems have technical advantages over conventional laparoscopic surgery that overcome the limited manual dexterity of laparoscopic instruments and provide ambidexterity in narrow space. Especially, robotic systems make it easy to dissect left side of pelvic cavity with the surgeon’s right or left hand. In addition, strong and steady traction with robot arms and self-controlled camera system enables an operator to secure a clear view. Dissection of the lower part of the rectum using robotic systems could be helpful in gaining access to the operative field in any direction, allowing excellent visibility for determining the relationship of the lower rectum to the levator ani muscle, the presacral fascia to the fascia propria of the rectum, and seminal vesicle or vagina to Denonvilliers’ fascia [12]. Neurovascular bundles are also clearly visible from the pelvic plexus and are meticulously dissected from the rectum [12]. In particular, it is difficult to dissect to near the anal canal in case of narrow and crooked pelvic cavity using laparoscopy. Robotic systems allowed precise and sharp dissection near the anal canal or up to anus in pelvic phase, therefore the duration of perineal phase was shorter in robotic surgery than in laparoscopic surgery [3].
We hypothesized that laparoscopically experienced surgeon was adequately prepared to perform safe and efficacious ISR by robotic approach, even at an early period of experience.
In one study, the first plateau of laparoscopic rectal resection was observed after 90 cases in learning curve for operating time [11]. Whereas, some studies reported the learning curve for robotic rectal surgery reached a first plateau after 17-22 cases [3,10]. In addition, Kim et al. [13] reported that, in terms of operating time, laparoscopically inexperienced surgeon who has sufficient open surgical experience and anatomic knowledge can adapt to robotic procedure after 20 cases without increase of postoperative complication. Our study showed that operating time in robotic ISR was comparable to those in laparoscopic ISR for just less than 20 cases. Previous studies reported that robotic procedures tended to take longer in operating time [3,6,10,14,15]. The other studies including systemic review and meta-analysis, whereas, reported that there were no significant differences in operating time [16,17]. In present study, total operating time did not significantly differ between laparoscopic and robotic group, even after involving the time used for docking in robotic group. In general, robotic systems required time consuming procedures such as robotic arm docking and arrangement of instrument preventing collision [12]. Standardized protocol and accumulated experience for setting of robotic systems could reduce these times.
Oncologic adequacy was assessed by LN clearance, circumferential margin clearance and distal margin clearance. In our study, the number of LN harvested and distal margin clearance were similar to previously reported studies [3,8,9]. Circumferential margins of both groups were similar to previous studies [3,7,8,18]. However, circumferential margin positive was identified in three patients (15.8%) in both groups, which showed relatively high positive rate compared with other studies [3,8,18]. All patients in robotic group were stage T4. All patients in laparoscopic group were stage T3 and tumors were located within 3 cm from anal verge. High positive rate of circumferential margin in our study was considered due to the small number of patients enrolled.
This study has some limitations. It is a retrospective study of prospectively collective data, which has inherent selection bias. In addition, there is a lack of data on urologic and sexual function, which may have reflected the quality of rectal dissection. However, to the best of our knowledge, there are few studies comparing robotic and conventional laparoscopic ISR for low rectal cancer. Based on the results of the present study, a longer follow-up could be required to assess the long-term outcomes of local recurrence and cancer-free survival.
In conclusion, our results suggest that robotic ISR is a safe and feasible procedure for low rectal cancer and showed comparable outcomes with laparoscopic surgery. All operations were performed by a single surgeon who already has highly experienced laparoscopic rectal surgery. Especially, operating time in robotic ISR showed comparable to those in laparoscopic ISR for just less than 20 cases. This suggests that, for a skilled laparoscopic surgeon, robotic systems can contribute to reduce the technical difficulties of rectal resection without the requirement of a long learning time. In addition, recent studies reported that robotic surgery could provide an enhanced benefit to patients in the management of mid to low rectal cancer in terms of postoperative recovery and functional outcomes [3,19]. Although our results showed only comparable outcomes between robotic and laparoscopic surgery, it is expected that the superiority of robotic surgery will be proved if the large scale of the study is in progress.
Notes
No potential conflict of interest relevant to this article was reported.