INTRODUCTION
Colorectal cancer is one of the most occurring malignancies, and the incidence is expected to increase in Korea with the aging population and westernized lifestyles [1]. Based on data from Korea Central Cancer Registry, the incidence rate of colorectal cancer increased from 20.7 (men, 22.5 and women, 18.9) per 1,000,000 in 1999 to 54.9 (men, 65.1 and women, 44.7) per 1,000,000 in 2017 [2]. Early diagnosis and proper management are the most important in the treatment of colon cancer. When it is resectable, colon cancer can be managed with surgery only, or surgery with adjuvant chemotherapy whereas rectal cancer requires surgery only in early stage or surgery with neoadjuvant or adjuvant chemoradiation in advanced stage. In addition, the survival rate for colorectal cancer have been improved due to the recent increase of early diagnosis, improvement in surgery, development of chemotherapy agent, and improvement of neoadjuvant chemoradiation treatments. The 5-year survival rate of colorectal cancer in Korea was also improved from 54.8% in 1995 to 74.8% in 2012 [1]. However, there have been few recent reports on the survival rate of colorectal cancer in Korea.
The aim of this study was to evaluate the clinical characteristics and oncologic outcomes of colorectal cancer patients who underwent curative surgery followed with or without adjuvant chemotherapies.
METHODS
Patients
We reviewed the medical records of patients who underwent radical surgery for pathologically proven primary colorectal adenocarcinoma between 2009 and 2018 in National Health Insurance Service Ilsan Hospital, Goyang, Korea. Patients who underwent palliative resection or bypass surgery were excluded from this study. Patients with Tis (carcinoma in situ) adenocarcinoma and other colorectal cancer except adenocarcinoma such as lymphoma, sarcoma, and gastrointestinal stromal tumor were also excluded. This study was reviewed and approved by the institutional review board (IRB No. NHIMC 2018-09-010). The medical records of the patients were collected and reviewed retrospectively to evaluate the patients’ characteristics, operative data and survival outcomes.
Colorectal cancer was divided into colon cancer and rectal cancer, and the rectosigmoid colon cancer was classified into colon cancer. Colon cancer can be subdivided to appendiceal cancer, cecal cancer, ascending colon cancer, hepatic flexure cancer, transverse colon cancer, splenic flexure cancer, descending colon cancer, sigmoid colon cancer, and rectosigmoid colon cancer according to the anatomic location. Colon cancer located from appendix to transverse colon was categorized as right-side colon cancer and colon cancer from splenic flexure colon to rectosigmoid colon was categorized as left-side colon cancer in this study.
The analysis included sex, age, name of operation, date of operation, pathologic stage, preoperative carcinoembryonic antigen (CEA) levels, associated polyp, tumor differentiation, recurrence and survival. Tumor stages were determined according to the American Joint Committee on Cancer (AJCC) staging, 8th edition. Postoperative death was defined as death within 30 days from surgery.
Statistical analyses
All statistical analyses were performed using SAS statistical software version 9.3 (SAS Institute Inc., Cary, NC, USA). The results were presented as means with standard deviations (mean±SD) for continuous outcomes, and as frequencies and percentages for categorical outcomes. Categorical variables were compared using chi-square or Fisher exact tests, and continuous variables were compared using independent sample t-tests. The survival rate was estimated by the Kaplan-Meier method and compared by the log-rank test. Multivariate analyses were performed by using Cox’s proportional hazards model to identify prognostic factors. P-value of less than 0.05 was considered statistically significant.
RESULTS
Between 2009 and 2018, 1,126 patients underwent radical surgery for colorectal adenocarcinoma, and Table 1 summarizes patients’ characteristics. Of these patients, 683 patients (60.7%) were males, and there were 18 patients under the age of 40 (1.6%), 404 patients of the age between 41 and 65 years old (35.9%), and 704 patients (62.5%) aged 65 years old or older. By stage, there were 241 patients (21.4%) in stage I, 382 patients (33.9%) in stage II, 392 patients (34.8%) in stage III, and 111 patients (9.9%) in stage IV. The preoperative CEA level was more than 5 ng/dL in 276 patients (27.2%). The preoperative colonoscopy identified associated polyps in 44.2% of patients (colon cancer, 48.2% and rectal cancer, 38.2%). According to tumor differentiation, moderate differentiation type was the most common with 688 patients (65.7%). According to the anatomic location, right-side colon cancer, left-side colon cancer, and rectal cancer were found in 307 patients (27.2%), 441 patients (39.2%), and 378 patients (33.6%), respectively. Of these patients, four patients died within 30 days from surgery (mortality rate, 0.4%), and the causes of death were two respiratory failures, one cardiac shock, and one liver failure who underwent neoadjuvant chemoradiation for rectal cancer.
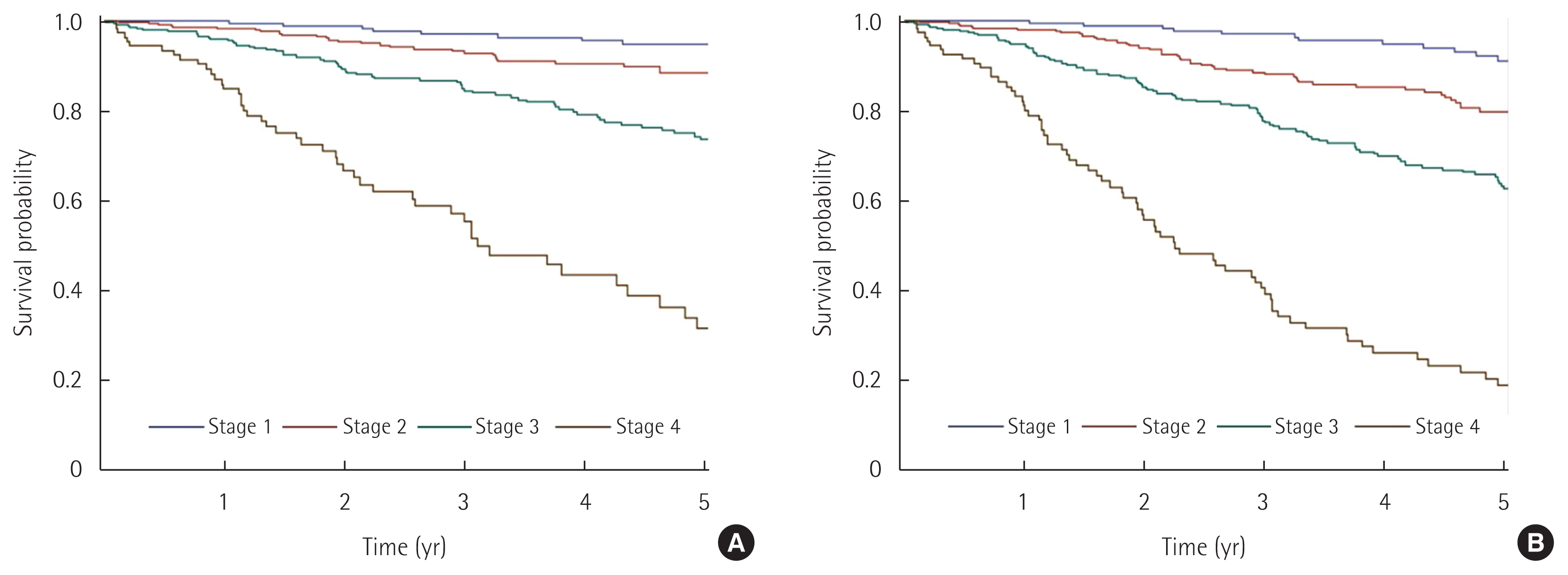
The median follow-up duration was 36.3 months (range, 0.1–120.3 months). During the follow-up period, 158 patients (14.0%) out of 1,126 patients died. These 158 patients included 114 colon cancer patients out of 745 patients (15.3%), and 44 rectal cancer patients out of 381 patients (11.5%). The recurrence occurred in 216 patients out of 1,126 patients (19.2%) including 136 patients (18.2%) with colon cancer, and 80 patients (21.0%) with rectal cancer. Of these recurrences in rectal cancer, local recurrence accounted for nine patients (2.4%), and there was no local recurrence in patients with colon cancer. Overall 5-year survival was 79.5%, and 5-year disease-free survival was 69.9%. Overall 5-year survival was significantly higher in rectal cancer than colon cancer (84.2% vs. 76.9%, P=0.014), whereas there was no significant difference in 5-year disease-free survival between colon cancer and rectal cancer (69.8% vs. 70.2%, P=0.338). Overall 5-year survival rates and 5-year disease-free survival rates according to stage were 94.7% and 91.0% in stage I, 88.4% and 79.8% in stage II, 74.3% and 63.3% in stage III, and 31.5% and 18.9% in stage IV (Fig. 1). Overall survival and disease-free survival were significantly higher in female patients than male patients (P=0.029 and P=0.041, respectively). The overall 5-year survival (P=0.001) and 5-year disease-free survival (P=0.014) were lowest in patient under 40 years old with 62.5% and 52.1% whereas highest in patients aged 41 to 65 years old with 86.5% and 74.9%. There was significant difference in overall 5-year survival and 5-year disease-free survival rate according to preoperative CEA level (P<0.001, both). Overall 5-year survival and 5-year disease-free survival rate in patients with poorly differentiated type were 54.9% and 32.7%, and there were statistical significances (P<0.001, both). Multivariate analysis revealed that male sex, elevated preoperative CEA level, and poorly or mucinous differentiation were poor prognostic factors for overall survival, whereas elevated preoperative CEA level, poorly or mucinous differentiation and presence of lymphovascular invasion were poor prognostic factors for disease-free survival (Tables 2, 3).
DISCUSSION
Various kinds of treatments have been developed with advance in basic research, clinical study, and research of carcinogenesis for colorectal cancer and their effectiveness has been reported in various ways [3–6]. Efforts to predict the prognosis and recurrence of colorectal cancer have been developed, but to date, the most powerful predictor of patients’ prognosis is TNM stage. The current stage of colorectal cancer is a combination of depth of invasion (T), lymph node metastasis (N), and distant metastasis (M) by AJCC classification system, which was also used in this study [7].
The incidence of colorectal cancer in Korea has increased remarkably during the past few decades [2]. Accordingly, the treatment of colorectal cancer, especially in advanced and metastatic cancer, has advanced and the result of treatment has improved. The survival rate by the AJCC system has been reported more than 90% in stage I, 70% to 85% in stage II, 25% to 80% in stage III, and less than 10% in stage IV [8,9]. In this study, overall 5-year survival rate was 79.5%, and 5-year disease-free survival rate was 69.9%. The overall 5-year survival rate by stage was 94.7% in stage I, 88.4% in stage II, 74.3% in stage III, and 31.5% in stage IV, which is more favorable compared to previous literatures, 5-year disease-free survival was 91.0% in stage I, 79.8% in stage II, 63.3 in stage III, and 18.9% in stage IV. Jung et al. [1] reported frequency, mortality, and survival rate of colorectal cancer based on data of the Korea National Cancer Incidence Database in 2015. Colorectal cancer was the fourth most common cause of death in men and second in women. They reported that the survival rate for patients with colorectal cancer between 2008 and 2012 was 74.8% (76.9% in male patients and 71.8% in female patients) and the survival rate has improved compared to the past periods. The survival rate of 79.5% (76.4% in male patients and 84.7% in female patients) may be regarded as improving results over time.
Lee et al. [10] reported the survival rate in 689 patients with colorectal cancer according to subside of colon and rectum, which showed overall 5-year survival rate of 77.8% including 92.9% in cecal cancer, 69.5% in ascending colon cancer, 76.2% in transverse colon cancer, 84.0% in descending colon cancer, 82.2% in sigmoid colon cancer, and 77.5% in rectal cancer. In the United States, about 145,600 patients are diagnosed as colorectal cancer per year including 101,420 patients with colon cancer and 44,180 patients with rectal cancer. Overall 5-year survival rates for these patients were 65%, including 90% for localized disease, 71% for regional disease, and 14% for distant disease. In addition, overall 5-year survival rates for colon cancer was 64%, including 90% for localized disease, 71% for regional disease, and 14% for distant disease while overall 5-year survival rates for rectal cancer was 67%, including 89% for localized disease, 71% for regional disease, and 15% for distant disease [11]. These results are similar to the data between 2009 and 2015 which showed overall 5-year survival rates of 63% for colon cancer, including 90% for localized disease, 71% for regional disease, and 14% for distant disease while overall 5-year survival rates of 67% for rectal cancer, including 89% for localized disease, 71% for regional disease, and 15% for distant disease [12]. However, the overall 5-year survival and 5-year disease-free survival for distant disease in our study were 31.5% and 18.9%, respectively. Recent aggressive surgical treatment and advanced chemotherapy regimen for metastatic colorectal cancer seem to have improved the survival rate.
As an aging society progresses, there is a growing interest in colorectal cancer surgery in elderly patients. According to Seow-En et al. [13] who reported surgical outcomes in patients with advanced age, median overall survival was 78 months. Following multivariate analysis, the factors significant for predicting overall mortality were serum albumin <35 g/dL, serum CEA ≥20 μg/L, T stage 3 or 4, moderate tumor cell differentiation or worse, mucinous histology, rectal tumors, and preexisting chronic obstructive lung disease. However, advanced age alone was not found to be significant. In our study, we divided the age group into 40 years old and younger, 41 to 64 years old and 65 years old or older. The age group of 40 years old and younger had the lowest overall 5-year survival rate of 6.25% and overall 5-year survival of 75.7% in 65 years old and older group was similar to previous literatures.
Various factors such as tumor stage, preoperative CEA, cell differentiation, vascular invasion, intestinal obstruction, intestinal perforation, age, and sex have been reported as predictive factors on survival rate following curative resection for colorectal cancer [14–16]. In our study, there was significant difference in survival rate according to tumor stage, preoperative CEA, age, and sex. Recurrence rate after curative resection for colorectal cancer has been reported as 30% to 50% [17]. Ryuk et al. [16] defined early recurrence as recurrence within 2 years after curative resection. The liver was the most common site of early recurrence (40.5%), whereas late recurrence was more common locally (28.1%), or in the lung (32.8%). The 5-year overall survival rates for early and late recurrence were 34.7% and 78.8%, respectively. The recurrence rate in our study was 19.2%.
Tekkis et al. [18] reported the 30-day mortality of 7.5% in 8,077 patients with colorectal cancer. They suggested age, American Society of Anesthesiology grade, Dukes’ stage, and emergency operation as independent risk factors for mortality. Rutegard et al. [19] reported that mortality within 30 days of surgery decreased from 2.1% in 2000–2003 to 1.6% in 2008–2011. Although the mortality rate varies by reporters, postoperative mortality is still a major issue of concern. To improve the survival rates, low mortality rate could also be a point to consider. With improvement of surgical skills as well as medical supports, the mortality rate is expected to become lower. The postoperative 30-day mortality in our study was 0.4%. Although we did not analyze the risk factors for the 30-day mortality because of the low rate of mortality, surgeons should pay a great attention to avoid the mortality in the perioperative period.
With the development of surgical skills and various treatments, postoperative outcome of colorectal cancer is expected to improve. It may be helpful for surgeons to improve their surgical outcomes when they review their data and conduct active researches.